Women’s health

Women’s health

Women’s health
This section provides learning modules with CPD credits for obstetricians and gynaecologists, gynaecology specialist nurses, hospital doctors, genitourinary medicine specialists and other healthcare professionals, across a range of topics in women’s health, including but not limited to menstrual disorders, cancers, perinatal health, adolescent gynaecology, contraception, menopause and hormonal therapy and a monthly round-up of the latest research studies and how they could inform clinical practice.
Mr Abdelmageed Abdelrahman
Consultant in gynaecology and subspecialist in urogynaecology and clinical adviser to MIMS Learning

Sexual assault and forensic gynaecology


Module description
1 CPD hour
This learning module by Professor Rudo Masanzu advises on what action to take following a disclosure of rape or sexual assault, including an immediate safety assessment, forensic considerations and ongoing support for the patient.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Understand the legal definitions of rape and sexual assault
● Consider the initial approach to, and management of, a person who discloses a sexual assault
● Discuss the principles of forensic medical examinations and evidence gathering
● Describe injuries using correct forensic terminology
Scope of the problem
The volume of sexual offences recorded by the police has been increasing over the last decade, and for the year ending March 2022 there were 193,566 police recorded offences.
Data on the prevalence of rape and sexual assault in England and Wales reveal:1–3
● Some 20% of women have experienced a sexual assault since the age of 16 years. One in four women have been raped or sexually assaulted as an adult, and globally this rises to one in three.
● Some 4% of men have experienced a sexual assault since the age of 16 years. One in 18 men have been raped or sexually assaulted as an adult.
● At least 15% of girls and young women and 5% of boys and young men are sexually abused before the age of 16 years.
However, there is widespread underreporting and only 10–15% of sexual offences are ever reported to the police. Instead, victims may present to their GP, to a sexual health clinic or to advocacy services to seek help and support.
One in four women have been
raped or sexually assaulted as an adult.
(Image credit: Pixelfit/Getty Images)
References
1. Centre of Expertise on Child Sexual Abuse (CSA Centre). The scale and nature of CSA. Accessed June 2023.
2. Crime Survey for England and Wales (CSEW). Accessed June 2023.
3. Office of National Statistics. Sexual offences in England and Wales overview: year ending March 2022. Accessed June 2023.

Scope of the problem
The volume of sexual offences recorded by the police has been increasing over the last decade, and for the year ending March 2022 there were 193,566 police recorded offences.
Data on the prevalence of rape and sexual assault in England and Wales reveal:1–3
● Some 20% of women have experienced a sexual assault since the age of 16 years. One in four women have been raped or sexually assaulted as an adult, and globally this rises to one in three.
● Some 4% of men have experienced a sexual assault since the age of 16 years. One in 18 men have been raped or sexually assaulted as an adult.
● At least 15% of girls and young women and 5% of boys and young men are sexually abused before the age of 16 years.
However, there is widespread underreporting and only 10–15% of sexual offences are ever reported to the police. Instead, victims may present to their GP, to a sexual health clinic or to advocacy services to seek help and support.
One in four women have been
raped or sexually assaulted as an adult.
(Image credit: Pixelfit/Getty Images)
References
1. Centre of Expertise on Child Sexual Abuse (CSA Centre). The scale and nature of CSA. Accessed June 2023.
2. Crime Survey for England and Wales (CSEW). Accessed June 2023.
3. Office of National Statistics. Sexual offences in England and Wales overview: year ending March 2022. Accessed June 2023.

Legislation and definitions
The Sexual Offences Act 2003 (the Act) applies to England and Wales only and came into force on 1 May 2004. Scotland is covered by the Sexual Offences (Scotland) Act 2009, whilst Northern Ireland is covered by the Sexual Offences (Northern Ireland) Order 2008.
To summarise, the Act consists of three parts, in which Part 1 sets out the range of sexual offences, covering rape, assault by penetration, causing sexual activity without consent, sexual assault and causing a person to engage in sexual activity without consent.4 It covers child sex offences and offences involving an abuse of a position of trust towards a child. It also includes provisions on sexual offences against people with mental disorders, prostitution, trafficking, and preparatory offences.4

Sections of the Act include:
● Section 1: Rape (maximum sentence = life)
● Section 2: Assault by penetration (maximum sentence = life)
● Section 3: Sexual assault (maximum sentence = 10 years)
● Section 5: Rape of a child under 13 (maximum sentence = life)
● Section 6: Assault by penetration of a child under 13 (maximum sentence = life)
● Section 7: Sexual assault of a child under 13 (maximum sentence = 14 years)
The Act states that a person (A) commits the offence of rape if:
● he (A) intentionally penetrates the vagina, anus or mouth of another person (B) with his penis,
● that person (B) does not consent to the penetration, and
● (A) does not reasonably believe that (B) consents.
Assault by penetration is committed if a person (A) intentionally sexually penetrates the vagina or anus of another person (B) with a part of their body or anything else, and B does not consent to the penetration, and A does not reasonably believe that B consents.
For the purposes of the Act the term ‘vagina’ includes the vulva.
References
4. Legislation.gov.uk. Sexual Offences Act 2003. Accessed June 2023.
Injury terminology
Scroll within the image below to view an overview of types of injuries in terms of causation, and the correct forensic terminology to describe them.
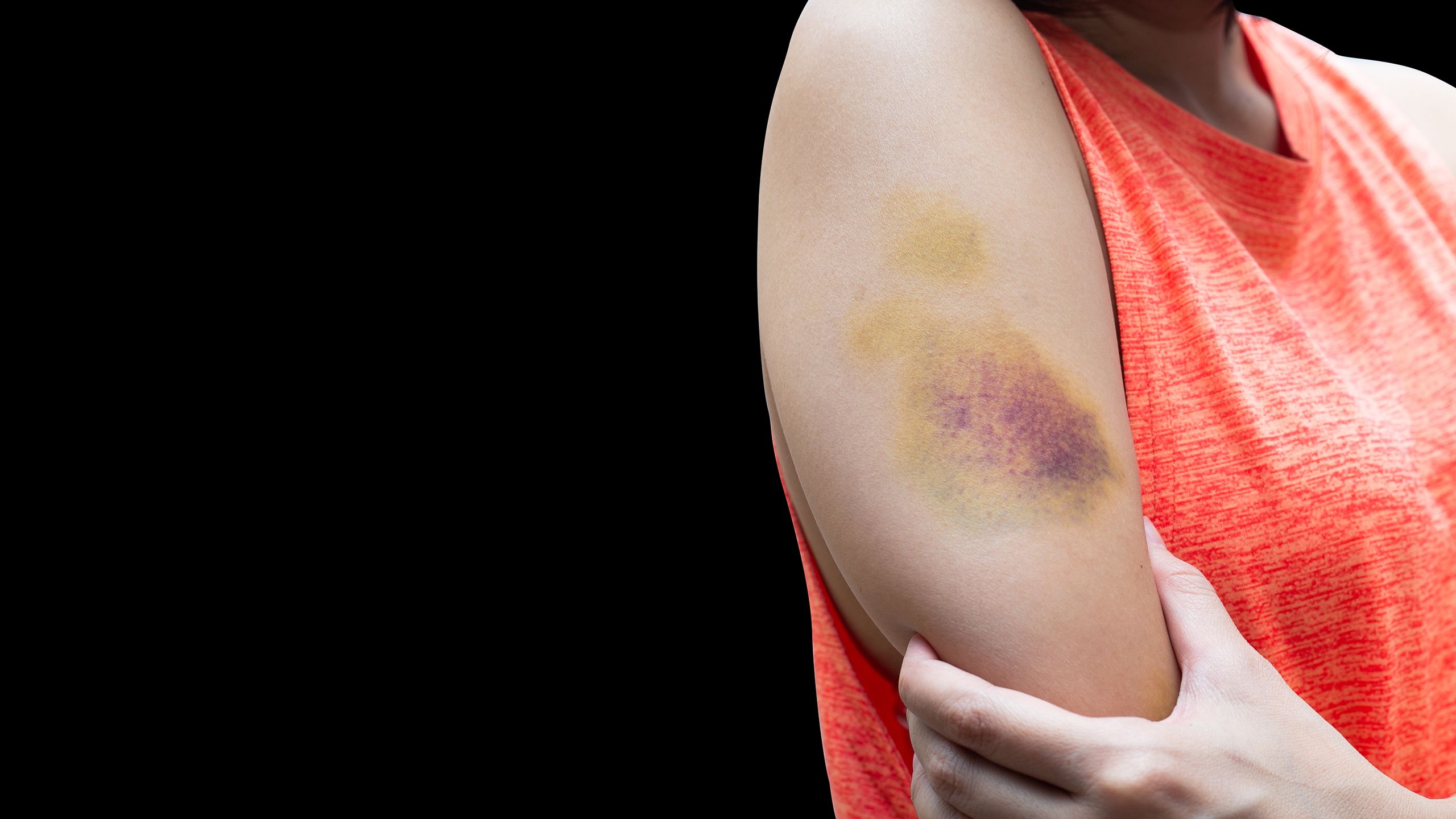

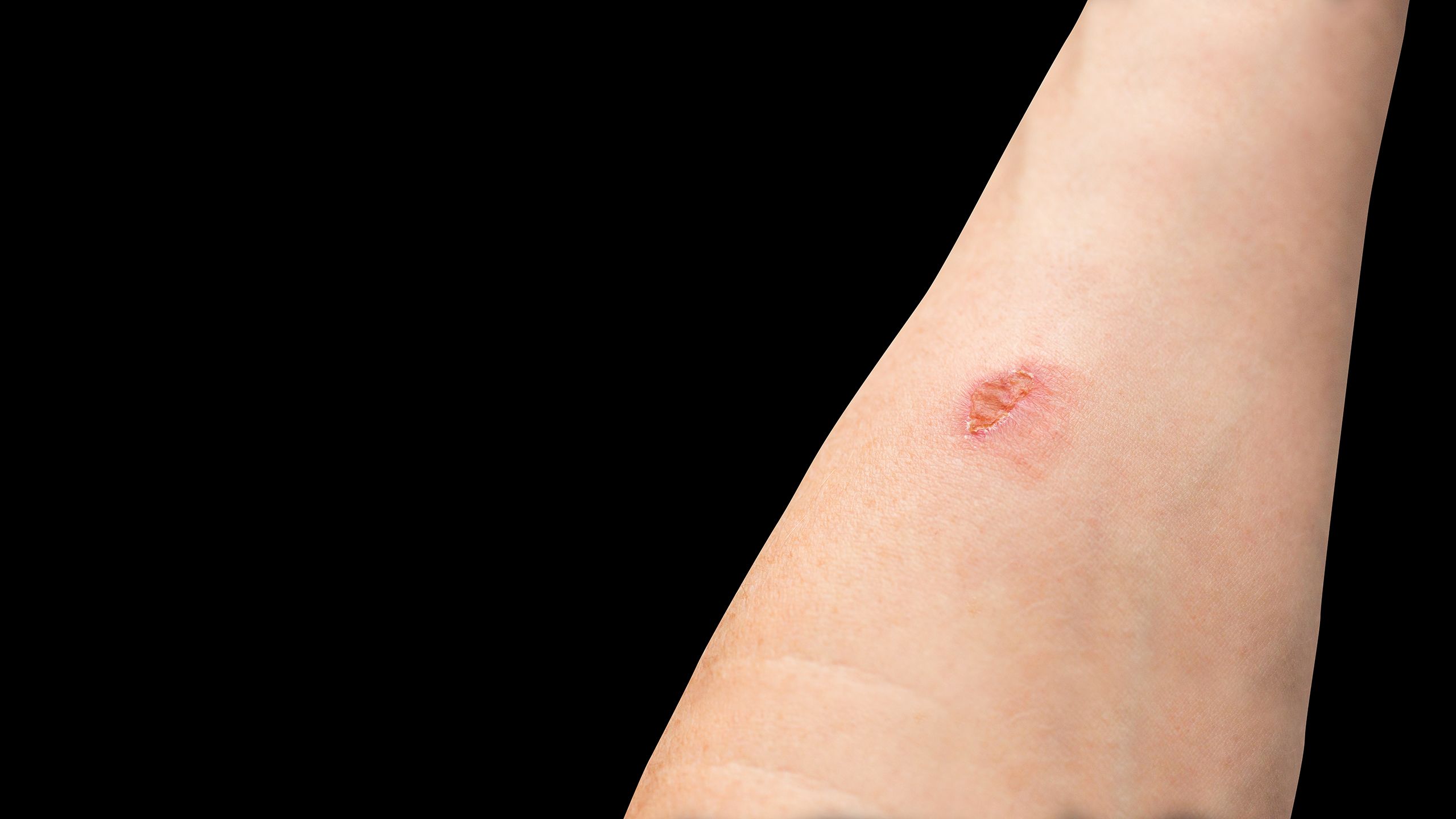
Injury causation
Blunt force
Forensic injury terminology
● bruise: includes petechiae (pin-point haemorrhages)
● patterned bruises: such as tramline bruises (for example, from a baton or rod)
● abrasion: lay terms are ‘graze’, ‘scratch’, ‘scuff injury’
● laceration: lay term is ‘tear’
Injury causation
Sharp force
Forensic injury terminology
● incision: lay term is ‘cut’
● stab/penetrating wounds
Injury causation
Other
Forensic injury terminology
● burns: caused by extremes of temperature, or can be electrical or chemical
● bites: may be human or animal
● erythema: lay term is ‘redness’
Terms such as ‘ecchymosis’ and ‘contusion’ are not used forensically. Only the term ‘bruising’ is used, which describes damage to blood vessels beneath the skin as a result of blunt force, pressure or a blow leading to leakage of blood into the surrounding tissues.
Erythema (redness of the skin or mucous membranes) is caused by an increase in blood flow to capillaries. It can occur with injury, infection, or inflammation. Erythema disappears on finger pressure (it is blanching), while bruising and pigmentation do not.
Sexual assault and forensic gynaecology
Read more about what action to take following a disclosure of rape or sexual assault, including conducting an assessment, screening for sexually transmitted infections and emergency contraception in this learning module.
Sexual assault and forensic gynaecology
Read more about what action to take following a disclosure of rape or sexual assault, including conducting an assessment, screening for sexually transmitted infections and emergency contraception in this learning module.

Heavy menstrual bleeding - red flag symptoms


Module description
0.5 CPD hours
This learning module, updated by Dr Toni Hazell, provides a refresher on red flag symptoms associated with heavy menstrual bleeding (menorrhagia). Key learning points for healthcare professionals include identifying when urgent referral is required.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● List the red flag symptoms of menorrhagia
● Understand possible causes
● Take a focused patient history
● Prescribe or refer to secondary care appropriately
This module has been updated to include the updated NICE guideline (NG88) on heavy menstrual bleeding.
Red flag symptoms
Menorrhagia is an excessive menstrual blood loss that interferes with a woman's social, emotional and/or material quality of life.
About 30% of patients describe their periods as `heavy’. Menstrual disorders are the second most common gynaecological condition, resulting in 12% of all gynaecology referrals.1
Red flag symptoms
● Persistent intermenstrual or postcoital bleeding.
● An unexplained vulval lump or vulval bleeding as a result of ulceration.
● A palpable abdominal mass that is not obviously uterine fibroids.
Reference
1. Duckitt K. Menorrhagia. BMJ Clin Evid 2015 Sep 18; 2015.


Red flag symptoms
● Persistent intermenstrual or postcoital bleeding.
● An unexplained vulval lump or vulval bleeding as a result of ulceration.
● A palpable abdominal mass that is not obviously uterine fibroids.
Reference
1. Duckitt K. Menorrhagia. BMJ Clin Evid 2015 Sep 18; 2015.
Possible causes
Around half of women with menorrhagia have dysfunctional uterine bleeding and do not have any underlying cause. Other possible causes are listed below.
● Uterine and ovarian pathologies: uterine fibroids, endometriosis and adenomyosis
● Pelvic inflammatory disease and pelvic infection
● Endometrial polyps, hyperplasia or carcinoma
● Polycystic ovary syndrome
● Systemic diseases and disorders: hypothyroidism, liver or renal disease
● Coagulation disorders such as von Willebrand disease
● Anticoagulant therapy
● Chemotherapy
● Intrauterine contraceptive device (blood loss may be increased by 40–50% over 6–12 months compared with pre-insertion values)
Rapid treatment of heavy bleeding
Oral norethisterone, 5mg three times a day for 10 days, usually stops bleeding within 1-3 days.1 A withdrawal bleed occurs 2-4 days after stopping treatment. This is equally as thrombogenic as combined hormonal contraception and should therefore not be used in women for whom combined hormonal contraception would be contraindicated for any reason. These women can use medroxyprogesterone.
If bleeding is exceptionally heavy ('flooding'), 10mg three times a day may provide better results but the patient needs to understand that this treatment carries an increased thromboembolic risk. This should then be tapered down to 5mg three times a day for about a week once bleeding has stopped.

Reference
1. Duckitt K. Menorrhagia. BMJ Clin Evid 2015 Sep 18; 2015.
Heavy menstrual bleeding - red flag symptoms
This learning module for GPs, gynaecologists and other clinicians provides a refresher on red flag symptoms associated with heavy menstrual bleeding (menorrhagia).
Heavy menstrual bleeding - red flag symptoms
This learning module for GPs, gynaecologists and other clinicians provides a refresher on red flag symptoms associated with heavy menstrual bleeding (menorrhagia).

Nausea and vomiting of pregnancy and hyperemesis gravidarum: clinical review


Module description
1.5 CPD hours
Dr Abdelmageed Abdelrahman gives an overview of severe nausea and vomiting of pregnancy, outlines the definition of hyperemesis gravidarum and explains when to consider inpatient management. Key learning points for healthcare professionals include suitable investigations and recommended antiemetic therapies.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Distinguish nausea and vomiting of pregnancy from hyperemesis gravidarum
● Use the Pregnancy-Unique Quantification of Emesis score to classify severity
● Identify key clinical features from the history
● Understand when to consider inpatient management
Prevalence
Nausea and vomiting of pregnancy (NVP) affects up to 80% of pregnant women.1 It is a common indication for hospital admission and typical admissions last three to four days.2
Hyperemesis gravidarum (HG) is the severe form of nausea and vomiting of pregnancy and affects 0.3–3.6% of pregnant women.1
Important!
Nausea and vomiting of pregnancy affects up to 80% of pregnant women
Reference
1. Einarson TR, Piwko C, Koren G. Quantifying the global rates of nausea and vomiting of pregnancy: a meta-analysis. J Popul Ther Clin Pharmacol 2013; 20(2): 171–83.
2. Lacasse A, Lagoutte A, Ferreira E, Bérard A. Metoclopramide and diphenhydramine in the treatment of hyperemesis gravidarum: effectiveness and predictors of rehospitalisation. Eur J Obstet Gynecol Reprod Biol 2009; 143: 43–9.



Prevalence
Nausea and vomiting of pregnancy (NVP) affects up to 80% of pregnant women.1 It is a common indication for hospital admission and typical admissions last three to four days.2
Hyperemesis gravidarum (HG) is the severe form of nausea and vomiting of pregnancy and affects 0.3–3.6% of pregnant women.1
Important!
Nausea and vomiting of pregnancy affects up to 80% of pregnant women
Reference
1. Einarson TR, Piwko C, Koren G. Quantifying the global rates of nausea and vomiting of pregnancy: a meta-analysis. J Popul Ther Clin Pharmacol 2013; 20(2): 171–83.
2. Lacasse A, Lagoutte A, Ferreira E, Bérard A. Metoclopramide and diphenhydramine in the treatment of hyperemesis gravidarum: effectiveness and predictors of rehospitalisation. Eur J Obstet Gynecol Reprod Biol 2009; 143: 43–9.
Diagnostic criteria
NVP should only be diagnosed when it occurs in the first trimester and other causes of nausea and vomiting have been excluded.
HG is diagnosed when there is protracted NVP with the following triad:



More than 5% pre-pregnancy weight loss
Dehydration
Electrolyte imbalance
Investigations
Investigations include urine dipstick (quantify ketonuria as 1+ or more) and MSU. Measure full blood count (to exclude infection and anaemia) and urea and electrolytes (to exclude hypokalaemia, hyperkalaemia, hyponatraemia, dehydration and renal disease). Check blood glucose.
An ultrasound scan may be needed to confirm viability and exclude multiple pregnancy or trophoblastic disease.

In refractory cases or in women with previous admissions, measure:
● TFTs to exclude hypothyroidism/hyperthyroidism
● LFTs to exclude liver disease
● Calcium and phosphate
● Amylase to exclude pancreatitis
● Arterial blood gas to exclude metabolic disturbances.
An ultrasound scan may be needed to exclude multiple pregnancy or trophoblastic disease
(Image credit: Science Photo Library/Getty Images)
Nausea and vomiting of pregnancy and hyperemesis gravidarum: clinical review
Dr Abdelmageed Abdelrahman gives an overview of severe nausea and vomiting of pregnancy for GPs, gynaecologists and other clinicians, outlining the definition of hyperemesis gravidarum and explaining when to consider inpatient management.
Nausea and vomiting of pregnancy and hyperemesis gravidarum: clinical review
Dr Abdelmageed Abdelrahman gives an overview of severe nausea and vomiting of pregnancy for GPs, gynaecologists and other clinicians, outlining the definition of hyperemesis gravidarum and explaining when to consider inpatient management.
Podcast: menopause interview with Dr Louise Newson
0.5 CPD hours
Benefit from learning tips that you can listen to any time, anywhere with the Clinical Update podcast. In this episode, Dr Louise Newson talks about menopause with MIMS Learning editor Pat Anderson. In other segments, MIMS Learning editors discuss key learning points from a module on chronic fatigue syndrome, and research on a dermatology topic very close to home.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Understand more about menopause management
● Demonstrate awareness of guidance on chronic fatigue syndrome
● Understand more about diagnosis of chronic fatigue
● Recall new dermatology research findings that affect children
Ovarian cancer: clinical review
1.5 CPD hours
This learning module by Dr Danielle Lindsay and Professor Sadaf Ghaem-Maghami covers the symptoms suggestive of ovarian cancer, how and when to investigate and how to provide information on the prognosis. Key learning points for healthcare professionals include clinical risk factors, investigation of serum CA125, and the psychosocial and psychosexual impact of ovarian cancer.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Understand the staging of ovarian cancer
● Describe the epidemiology of ovarian cancer
● Recognise patients with symptoms suggestive of ovarian cancer
● Initiate preliminary investigations and explain secondary care-based investigations
Safer prescribing for chronic conditions in pregnancy
1.5 CPD hours
In this module, Mr Abdelmageed Abdelrahman discusses the safety of prescribing in pregnancy. Key learning points for healthcare professionals include drugs to avoid during pregnancy and drugs that may more safely be used in treatment of chronic disease.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Understand the principles of prescribing in pregnancy
● Recall which drugs carry a risk of congenital malformation
● Safely prescribe for pregnant women with epilepsy, diabetes, depression, hypertension, and chronic kidney disease.
Complex contraception scenarios part 1
1.5 CPD hours
This case-based module by Dr Katie Boog and Dr Imogen Murray discusses contraception for specific patient populations. Scenarios covered in this module include contraception for young people, for transgender individuals, for those with obesity and for those who are taking other regular medications. The next module, Complex contraception scenarios part 2, covers contraception after pregnancy and for older individuals. The other module in this series is Contraception: the basics.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Help individuals with specific characteristics decide on the most suitable contraception for them
● Find guidance on the safety and effectiveness of contraception in complex scenarios
● Be aware of how contraception may interact with other drugs
Podcast: menopause interview with Dr Louise Newson
0.5 CPD hours
Benefit from learning tips that you can listen to any time, anywhere with the Clinical Update podcast. In this episode, Dr Louise Newson talks about menopause with MIMS Learning editor Pat Anderson. In other segments, MIMS Learning editors discuss key learning points from a module on chronic fatigue syndrome, and research on a dermatology topic very close to home.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Understand more about menopause management
● Demonstrate awareness of guidance on chronic fatigue syndrome
● Understand more about diagnosis of chronic fatigue
● Recall new dermatology research findings that affect children
Ovarian cancer: clinical review
1.5 CPD hours
This learning module by Dr Danielle Lindsay and Professor Sadaf Ghaem-Maghami covers the symptoms suggestive of ovarian cancer, how and when to investigate and how to provide information on the prognosis. Key learning points for healthcare professionals include clinical risk factors, investigation of serum CA125, and the psychosocial and psychosexual impact of ovarian cancer.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Understand the staging of ovarian cancer
● Describe the epidemiology of ovarian cancer
● Recognise patients with symptoms suggestive of ovarian cancer
● Initiate preliminary investigations and explain secondary care-based investigations
Safer prescribing for chronic conditions in pregnancy
1.5 CPD hours
In this module, Mr Abdelmageed Abdelrahman discusses the safety of prescribing in pregnancy. Key learning points for healthcare professionals include drugs to avoid during pregnancy and drugs that may more safely be used in treatment of chronic disease.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Understand the principles of prescribing in pregnancy
● Recall which drugs carry a risk of congenital malformation
● Safely prescribe for pregnant women with epilepsy, diabetes, depression, hypertension, and chronic kidney disease.
Complex contraception scenarios part 1
1.5 CPD hours
This case-based module by Dr Katie Boog and Dr Imogen Murray discusses contraception for specific patient populations. Scenarios covered in this module include contraception for young people, for transgender individuals, for those with obesity and for those who are taking other regular medications. The next module, Complex contraception scenarios part 2, covers contraception after pregnancy and for older individuals. The other module in this series is Contraception: the basics.
Educational objectives
After taking this activity healthcare professionals should be better able to:
● Help individuals with specific characteristics decide on the most suitable contraception for them
● Find guidance on the safety and effectiveness of contraception in complex scenarios
● Be aware of how contraception may interact with other drugs